Retinal Vascular Blockages
In the retina, as in the rest of the body, there are small blood vessels that bring blood into the retina (the arteries) and small blood vessels that bring blood out of the retina (the veins). If one of these blood vessels develops a blockage, the retina served by that vessel will not function normally, resulting in vision loss.
If the central artery or vein is blocked, the entire vision is affected. If a branch of the artery or vein is blocked, often a portion of the vision is affected. In many cases, no specific cause of these blockages are identified. Blood vessel blockages are more common in patients with high blood pressure, diabetes and in smokers. Certain tests may be necessary to look for blood cell abnormalities, blood vessel inflammation or other abnormalities in the cardiovascular system including the carotid arteries and heart. These tests may be critical in diagnosing and preventing other cardiovascular events.
Unfortunately, there is no proven way of reopening a blocked vessel to provide circulation and to repair the blocked retina. Unfortunately, this does not necessarily correspond to improved sight. Vision can sometimes be restored with intraocular or periocular injections, laser and occasionally vitrectomy surgery.
When a vein or artery is blocked, the retina is depleted of nutrients and oxygen which may cause the damaged retina to produce a growth factor which causes abnormal, friable blood vessels to develop. These abnormal blood vessels can lead to bleeding in the eye, retinal detachments and a severe type of glaucoma known as neovascular glaucoma. These conditions are more common with central retinal vein occlusions and can lead to sever vision loss, eye pain, nausea and vomiting and require prompt treatment. It is important to be monitored closely for at least six months for the development of these conditions as prompt treatment can often minimize the vision damage caused by the abnormal blood vessels.
Retinal Laser Surgery
Retinal laser surgery is an in office procedure commonly done by retinal physicians to treat retinal disorders such as diabetic retinopathy, retinal tears, macular edema (swelling) and retinal vascular occlusions.
Pneumatic Retinopexy
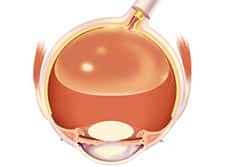
Pneumatic retinopexy is an in office procedure which involves injecting a small gas bubble into the eye with a hypodermic needle after topical or local anesthetic is applied to the eye. The procedure is used to repair superior (top of the retina) retinal detachments and is usually done in conjunction with laser or freezing (cryopexy) therapy to treat retinal tears in order to prevent recurrent retinal detachments after the gas is resorbed.
Vitrectomy
A common surgery performed for abnormal retinal conditions of the eye is called vitrectomy. The surgery involves removing the vitreous gel from the center of the eye. Abnormal vitreous is often a causative factor in the development of retinal diseases including diabetic retinopathy, macular pucker, macular hole and retinal detachments. The vitreous may also need to be removed first in order to get to retinal membranes, blood or scar tissue and to repair retinal detachments. The vitreous is replaced usually with saline (salt water), a temporary gas bubble or rarely, silicone oil.
Vitrectomy surgery is usually performed in our outpatient surgery center under local anesthesia with sedation. The surgery is done using a microscope and involves using small hypodermic needle sized instruments in the eye. The recuperation time can vary, but often, patients can return to work or normal activities in a week or two. Surgery requiring a gas bubble usually requires a month or longer to resume regular activities and may require postoperative head positioning for up to two weeks. Some complicated retinal disorders may require several surgeries.
All vitrectomy surgery has a risk of infection, bleeding, glaucoma, retinal detachment and further vision loss.
Scleral Buckle
Scleral buckle surgery is a procedure that is performed to repair a detached retina. This surgery is done in our outpatient surgical center or in the Newton Memorial Hospital Operating Room. The surgery is usually performed under local anesthesia with sedation. The recuperation time can vary, but patients can often return to work or normal activities within one or two weeks. Sometimes this procedure is done in conjunction with a vitrectomy in order to repair more complex retinal detachments and the recovery time would be longer in these cases. As with all retinal surgery, there is a risk of infection, glaucoma, retinal detachment, bleeding, need for further eye surgeries and irreversible vision loss.
B Scan Ultrasonography
An in office study that allows for diagnosing vitreous, retinal and choroidal disorders using sound waves when the back of the eye can’t be visualized with light and standard viewing instruments due to opacification such as a dense cataract or blood in the vitreous.
Optical Coherence Topography (OCT)
A special photographic study involving a state of the art optical system that quantitatively diagnosis’s and monitors macular edema (swelling) as well as other macular disorders. Response to treatment can also be followed with this equipment.
Fluorescein and Indocyanine Green Angiography
Fluorescein Angiography and Indocyanine Green Angiography (ICG) are in office diagnostic tests which are performed by injecting a special dye (Fluorescein/Indocyanine Green) into a vein of the arm or hand and taking a series of photographs with a special digital camera which employs filters.
The dye travels through the circulation and reaches the retinal and choroidal blood vessels. These tests allow great visualization of the blood vessels of the retina and choroid and are helpful in diagnosing and treating many retinal disorders, most commonly, macular degeneration, macular edema and diabetic retinopathy.
Intraocular/Periocular Injections
Injections of anti-inflammatory and anti-growth medicines are commonly used by retinal physicians to treat retinal disorders such as macular degeneration, diabetic retinopathy, macular edema (swelling), retinal vascular occlusions and ocular inflammations. The injections are done in the office and are given after topical (eye drops) anesthesia and occasionally local anesthesia are given. Minimal or no discomfort is usually reported by the patient after the procedure.

